Dr. Sanjay Gupta: After two years of Covid-19 vaccines, here’s why they’re still vital
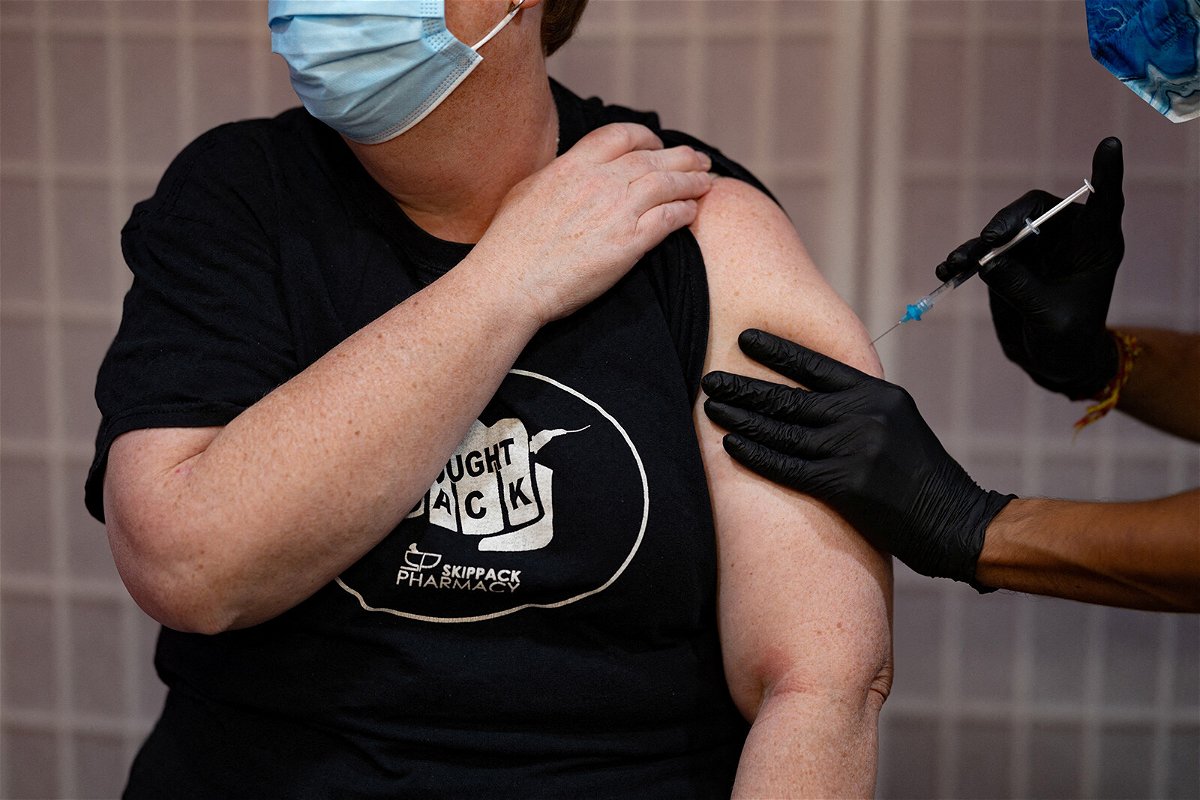
Amy Bagley
By Dr. Sanjay Gupta, CNN Chief Medical Correspondent
In the United States, approximately 658 million Covid-19 vaccine doses have been administered since they were first distributed exactly two years ago Wednesday.
Framing the significance of preventive measures like vaccines can be challenging, which is why a new report from the Commonwealth Fund and Yale School of Public Health made headlines: According to their modeling of disease transmission across all age demographics and taking into account the existing health conditions in so many Americans, Covid vaccines prevented an estimated 3.2 million deaths and 18.5 million hospitalizations from their introduction in December 2020 to November 30, 2022.
That is why it is surprising to hear, according to a Kaiser Family Foundation analysis of data from the US Centers for Disease Control and Prevention, that from April through August — the last month included in the analysis — there were more vaccinated than unvaccinated people dying of Covid. The vaccinated categories include people who were vaccinated with the primary series and people who had been vaccinated and received at least one non-bivalent booster.
According to a CNN analysis of additional CDC data for September, 12,593 people died of Covid. A CDC sample of the deaths found 39% were unvaccinated, and 61% were vaccinated.
This phenomenon has many people — especially vaccine skeptics, but even stalwart vaccine supporters — confused and wondering if Covid vaccines and boosters are still effective and warranted.
The short answer is yes — but understanding why requires a crash course in statistics. We enlisted the help of Jeffrey Morris, a professor and the director of the Division of Biostatistics at the Perelman School of Medicine at the University of Pennsylvania, who helped us define three key reasons more vaccinated than unvaccinated people are dying of Covid.
Statistics, part 1: base rate fallacy
One of the main reasons we see more vaccinated than unvaccinated people dying of Covid is a basic one. At this point in time, there are simply many more people who are vaccinated.
Think of it like this: If we round the September deaths to 13,000 and use the CDC sampling percentages, approximately 7,800 were vaccinated and approximately 5,200 were unvaccinated. The conclusion might be that you are far more likely to die if you are vaccinated. And, mathematically that would be true based on the raw numbers alone. If you stopped your analysis at this point, you will have committed a statistical error known as a base rate fallacy.
If instead, you take the extra step of accounting for the total number of fully vaccinated adults 18 and older in the United States (around 203 million) versus the total number of unvaccinated adults (around 55 million), a very different picture emerges.
Among the vaccinated population, 7,800/203 million died in September, which equals a rate of 38 deaths for every 1 million people. For the unvaccinated population, 5,200/55 million died, which equals a rate of 95 deaths for every 1 million people. That means an adult who is unvaccinated is roughly 2.5 times more likely to die than one who is vaccinated.
“You have to take into account the size of those groups,” explained Morris, who also publishes a blog, COVID-19 Data Science, to “just communicate what the emerging data suggest.”
Statistics, part 2: Simpson’s paradox
There is another important difference when looking at the vaccinated versus unvaccinated populations in the United States. The vaccinated population skews older and has more health conditions. These are the same groups that are much more likely to have worse outcomes, like hospitalization and death, when infected with SARS-CoV-2, the virus that causes Covid-19. For example, CDC data show more than 90% of deaths through mid-November have been in those 65 or older.
“So those things lead to a higher risk of death and also a higher probability of being vaccinated,” Morris said. “That’s the key: if the vaccine uptake of those high-risk groups is high enough, then we can have a majority of the hospitalized or fatal cases be higher in the vaccinated population.”
You are more likely to die if you are older, and also more likely to be vaccinated if you are older. It does not mean vaccination is more likely to lead to death.
So if age isn’t taken into account when assessing vaccine efficacy, it can lead to something known as Simpson’s paradox, where a trend can appear to be the opposite of reality.
Morris said those kinds of errors not only result in a serious underestimation of the benefit of vaccines but also to downright wrong conclusions, even flipping the results — in this case, making it appear that vaccines increase the risk of death.
This happened in August 2021, with a study out of Israel — a highly vaccinated country — showed 60% of those hospitalized with severe Covid were fully vaccinated, causing misinterpretation and raising questions about the continued value of vaccination.
Morris said he has also seen Simpson’s paradox when people look at the rate of Covid deaths before vaccines were rolled out in 2020 versus since then, or comparing countries with higher vaccination rates to countries with lower vaccination rates.
“It’s a lot more subtle, but the pandemic has provided a number of pure examples of it. So the bottom line with all of that is, we can’t accurately assess the effects of vaccines from simple summaries,” Morris said, however “seemingly intuitive” they may appear.
What the numbers show
A more telling and accurate comparison is between the death rate per 100,000 among unvaccinated people compared to the death rate of vaccinated people, adjusted for age.
CDC data show that for the week of September 25, people age 12 and older who were unvaccinated had a death rate of 1.32 per 100,000. Those who were vaccinated (but without an updated, bivalent booster) had a death rate of 0.26 per 100,000. And those who were vaccinated and boosted had a death rate of 0.07 per 100,000.
Broken down further by age, the numbers are even starker: The death rate during that week for those in the oldest age group, 80 and above, was 14.16 per 100,000 for the unvaccinated, 3.69 for those who were vaccinated but had not received the bivalent booster, and 0.0 for those who were vaccinated and boosted.
Overall, the CDC estimates that for the whole month of September, among those 12 and older, there was an almost 15 times lower risk of dying from Covid-19 for the vaccinated and boosted compared to the unvaccinated.
Unfortunately, uptake of the booster is low: Only 13.5% of the US population 5 and older is vaccinated and has gotten the new updated (bivalent) booster. Among those 65 and older, that percentage is 34.2%.
It’s not to say that vaccines are entirely risk free. For example, in people — especially males — between the ages of 5 and 39, there were 224 verified cases of myocarditis or pericarditis, inflammation of the heart and lining, reported to the CDC after vaccination with an mRNA vaccine between December 14, 2020, and May 31, 2022. But that was out of almost 7 million vaccine doses administered.
A study examining those figures found myocarditis/pericarditis occurred within seven days approximately 0.0005% of the time after the first dose, 0.0033% of the time after the second dose of the primary series, and 0.002% after the first booster — but it varied by age and sex, and was much more common among 16- to-17-year-old males after a second shot or a booster.
According to a separate analysis of nearly 43 million people in England, the researchers found that for younger men, the Moderna vaccine in particular had the highest rates of post vaccine myocarditis — although this number was still very low, 97 per million people exposed (0.0097%) — leading some to suggest a different vaccine for that age group or a longer interval between vaccine doses.
Waning immunity + new variants = lower efficacy
Statistical optical illusions aside, the fact is, there are more so-called breakthrough cases among the vaccinated. They have always existed. Since December 2020, we have known these vaccines are not 100% effective at preventing severe illness and death, let alone infection. When vaccines were first introduced, their efficacy was estimated to be an astonishing 95% against severe illness and death. They even protected people at a very high rate against infection.
But the efficacy keeps ticking downward. Part of it is waning immunity: Over the course of several months, antibody levels fade away — that’s just how the body works — even though there is still some protection, thanks to B cells and T cells. Getting boosted — or catching Covid — can help increase antibody levels for a few months at least. Between those two options, it’s far safer and less disruptive to get a booster than to risk illness.
Meanwhile, new variants keep cropping up, and they are increasingly able to evade our immune system. Unlike earlier variants, including the highly transmissible Delta variant, descendants of the Omicron lineage are escape artists.
“The emergence of Omicron at the end of 2021 was a game changer, as Omicron and its subsequent subvariants demonstrated strong immune evasion properties, with mutations in the spike protein and especially the [receptor binding domain] that reduced the neutralizing ability of the vaccine-induced antibodies,” Morris noted. The result is a great reduction in vaccine efficacy against infection, as well as against severe and fatal disease.
This actually means it’s more important to get boosted, especially if you are in a high-risk category, and as the weather gets colder and we gather indoors to spend time together.
The newest booster — the bivalent booster — is designed to protect against the original SARS-CoV-2 virus and against the more recent Omicron subvariants, although how much and for how long is still unknown.
Covid cases, and deaths have slowed down in recent months, but those numbers are trending up like they’ve done during the holidays in previous pandemic years. For the week of December 7, weekly new cases topped 65,000 and Covid claimed the lives of almost 3,000 people. Both represent an increase of around 50% from the week before, according to CDC data.
All of this is happening at a time when hospitals are already full of patients sick with the flu and RSV.
The bottom line
I know we’re all tired of hearing that we need to roll up our sleeves and get yet another Covid-19 booster.
But remember, many of us get the flu shot every year: We don’t assume we are protected from a flu vaccine a year ago. We get the shot even in seasons when the flu vaccine is much less effective than the Covid vaccine (the latest one appears to be a good match). We don’t call it a booster — it’s just the annual flu vaccine. And we don’t track the rate of so-called breakthrough flu infections; unlike Covid, we don’t routinely test people for flu unless they are demonstrably sick, so we have no way of knowing how many people, vaccinated or not, are infected and asymptomatic or mildly ill.
For some diseases, like measles, a single vaccine or a previous infection provides us with a near lifetime of protection. Even though we hoped for a one-and-done scenario when the Covid vaccines rolled out two years ago, the virus didn’t lend itself to that. Newer vaccines are being studied that could offer far more durable protection.
Analyzing all of this data without falling into the trap of a base rate fallacy or Simpson’s paradox isn’t easy, as you can see. And it is also clear the overall effectiveness of the vaccines have waned over time and with new variants.
However, two years later, a more thorough statistical analysis of vaccine effectiveness shows they are still cause for celebration.
The-CNN-Wire
™ & © 2022 Cable News Network, Inc., a Warner Bros. Discovery Company. All rights reserved.
CNN Health’s Andrea Kane and Deidre McPhillips contributed to this report.
